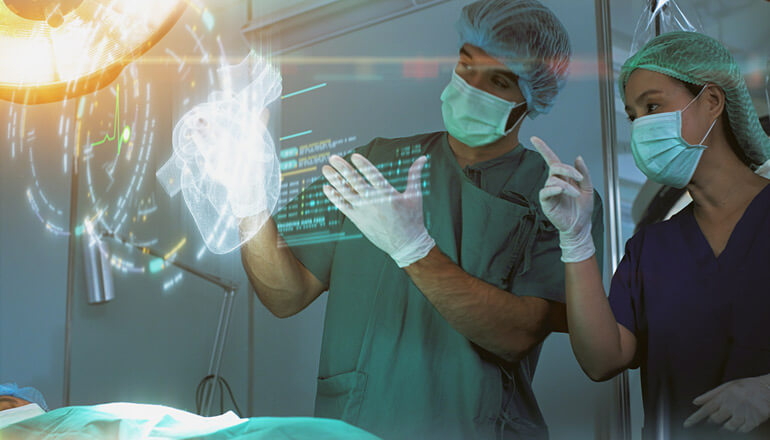
The good news for diabetics is that, though there’s no cure, diabetes technology is still advancing in the right direction. And with new devices, apps and big data leading the way, living with the disease is becoming a little bit easier. Here are some innovations making a big difference to patients.
Less-invasive glucose monitors
People with type 1 and type 2 diabetes have to carefully track their glucose levels. Traditionally, that has meant pricking their fingers with a needle to get a blood sample. But nowadays, diabetics can use a continuous glucose monitor instead.
The device is inserted under the skin, usually in the upper arm or the abdominal area, and provides real-time glucose measurements. Patients can set alerts to warn them if their blood sugar levels become dangerous. Some monitors can also connect to an insulin pump.
Companies are developing increasingly accurate monitors, and some manufacturers now provide patients with a history of their results, helping them gain a better understanding of their condition and what to watch out for. Patients can also upload information from their smartphones to the cloud, where doctors and nurses can see it.
Insulin delivery improvements
When diabetics do need glucose, they need it fast. In the past, their only options would have been painful injections or an insulin pump. But that is no longer the case — insulin can now be delivered through a less-invasive method using an inhaler.
Insulin pumps have advanced as well, simplifying how type 1 diabetics control blood sugar levels. In 2016, the U.S. Food and Drug Administration (FDA) approved the first automated insulin delivery device. The system checks glucose levels every five minutes and supplies the appropriate level of insulin when needed.
Surgical treatment advances
Fractyl, a manufacturer of surgical devices and the firmware and software that control them, is in the research and development phase of an experimental technique to facilitate the surgical treatment of patients with type 2 diabetes. Fractyl’s device and procedure, powered by Microsoft software and a custom application by Insight's Digital Innovation team, could have significant impact on the treatment of type 2 diabetes.
Pain relief without drugs
A high-frequency transcutaneous electrical nerve stimulation (TENS) device strapped around the calf can be used to ease or eliminate the pain of diabetic neuropathy. The device works by sending pulses that signal the brain to trigger the body’s natural pain relief response so drugs aren’t necessary. It’s especially helpful for people who are awakened at night by tingling or the sensation of burning feet. It could also help limit the need for opioids.
Apps for everything
Diabetics can use smartphone apps for everything from tracking calories to tracking glucose and weight. They can also record insulin levels, exercise habits and sugar intake. There’s even an app for diabetic-friendly recipes.
Revolutionizing research with big data
In addition to transforming medical research as a whole, big data has the potential to provide groundbreaking new insights into diabetes. With information gathered from multiple databases, researchers can more easily identify patterns in the population and conduct studies that are more robust.
Research discussed in the journal Big Data collected information from insurance claims, pharmacy records, healthcare providers and labs. It then used machine learning to develop predictive models and risk factors for the onset of type 2 diabetes. Scientists who developed the models say they are at least 50% better at predicting the disease than current methods.
Several organizations are already taking advantage of the opportunities provided by big data to make other discoveries. The Indiana Bioscience Research Institute, Eli Lilly and Company, Roche Diagnostics, the Regenstrief Institute and the Indiana University School of Medicine, are one such example. The group plans to collaborate on research by leveraging big data from shared databases to analyze diabetic populations, improve understanding of the disease and develop better treatments.
Accenture and Roche have also formed a collaborative partnership. Using the Accenture Intelligent Patient Platform to gather diabetes patient information, researchers can improve their understanding of the disease and enhance diabetes care by sharing data-driven analytics with partners and integrating the findings into current and future solutions.
The more information scientists have to work with, the more they will learn about treating and managing the disease. Someday, big data may enable medicine to truly beat diabetes.