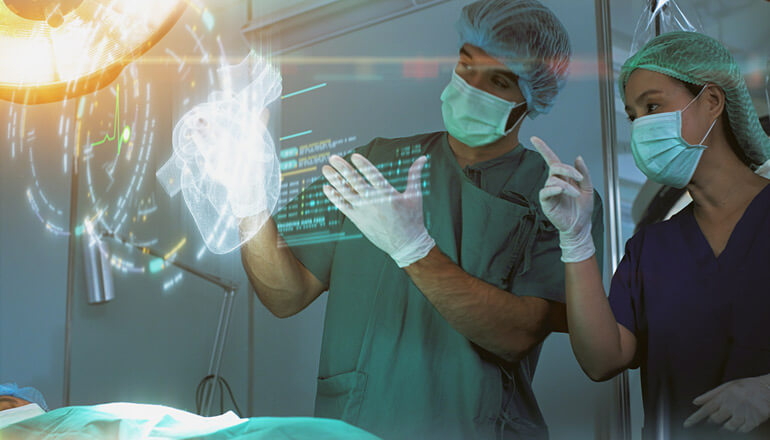
Thanks to emerging healthcare IT solutions, such as mobile devices and custom apps, patients can now speak with their physicians and even have a face-to-face consultation right from the comfort of their own homes.
But many healthcare organizations are just beginning to realize the bigger opportunities telehealth services open.
What is telehealth?
According to the American Telemedicine Association, telehealth encompasses a range of services, from health monitoring and patient consultation to the transmission of medical records. Telehealth is broadly associated with any type of electronic exchange of health information. Although the term telemedicine is often used interchangeably with telehealth, telemedicine is actually a subset of telehealth that refers more specifically to remotely provided clinical services designed to improve patient health.
A growing number of healthcare organizations in both the private and public sectors have embraced these kinds of services because of the game-changing benefits they provide to patients and clinicians. Telehealth has helped to not only expand and improve access to healthcare services, but also increase patient engagement and enable more efficient care models.
The Department of Veterans Affairs (VA), the largest integrated healthcare system in the United States, is also one of the largest providers of telehealth services. Last year, more than 700,000 veterans accessed VA telehealth services, which provide everything from mental healthcare to surgical specialist consultations.
In August, the VA announced it would further expand its telehealth services with the rollout of the VA Video Connect application, which enables veterans to access their providers through their personal computers or devices. The expansion also included the release of the Veteran Appointment Request app, a tool that enables veterans to use personal devices to schedule or change appointments at VA facilities. But it’s not just veterans who are benefiting from telehealth technology.
Improving healthcare access
One of the biggest advantages of telehealth services is that they make it easier for patients to access the care they need, when they need it. Nurse hotlines frequently help callers decide whether a condition can be treated at home or whether it necessitates immediate care. And who wants to drag themselves into the doctor’s office when they already feel miserable with a cold or flu? During a telemedicine consultation, a physician can just as easily inquire about symptoms, discuss treatment and determine whether a prescription is necessary.
More importantly, for patients who don’t have a reliable means of transportation or who struggle with mobility challenges or disabilities that make traveling difficult, remote access to a clinician can be a huge quality of life improvement. This is especially true for those living with chronic conditions for which frequent checkups are necessary.
Telehealth services are also helping to fill healthcare gaps faced by rural communities across the United States — in areas where patients may have to drive for hours to get to the nearest hospital or specialist. During a TEDx Talk in March, Lindsey Meyers, vice president of public relations at Avera Health, shared how a critically injured child was saved by a doctor more than 600 miles away. Through a video monitor, the doctor was able to guide local clinicians through reinflating the girl’s lungs and stabilizing her condition.
Telehealth systems that empower clinicians with on-demand remote access to critical care specialists have greatly helped improve job satisfaction for on-site caregivers.
“That’s powerful,” says Meyers. “It’s so powerful it extends the careers of our physicians in rural areas. New medical students pick sites with telemedicine over non-telemedicine sites for this reason. It’s become a recruitment tool.”
Lowering readmission rates
In-office visits and overnight stays at hospitals and skilled nursing facilities can be stressful and difficult for individuals in poor health. And if they’re suffering from multiple conditions, that can complicate care and make frequent hospital visits necessary. Even waiting rooms can expose patients to airborne illnesses, such as a cold or flu — pathogens that can prove fatal to elderly or immunocompromised individuals. For them, telehealth offers more than convenience; it’s a way to avoid unnecessary risk and protect their health.
Telehealth services reduce hospital readmission rates by enabling doctors to monitor patients more closely outside the office. Because of this, many hospitals have already started to include some form of remote monitoring as part of their post-discharge plans. By equipping patients with wearable devices or other wireless technologies, clinicians can monitor vital signs and symptoms and adjust post-release care as needed without requiring an in-office visit. This also encourages patients to become more actively engaged in their care outcomes.
Alignment Healthcare developed a program to remotely monitor chronically ill and recently discharged patients with the goal of reducing their 30-day readmission rates. Alignment extended the program to the sickest 10% of its patients. Enrollees were given a package of Bluetooth-enabled monitoring equipment, including a Samsung tablet, blood pressure cuff, pulse oximeter and scale. Patients were also trained on how to use all of the equipment in the package before being sent home.
According to a May article by Alignment’s Chief Medical Officer Ken Kim, the organization’s efforts have paid off. “Because of the program, Alignment’s seniors are seeing reduced 30-day readmission rates … compared to the national Medicare average readmission rate of about 18%. In 2016, Alignment members enrolled in remote [monitoring] across all markets saw hospital readmission rates of 7.2%,” he reported.
Making quality care more cost-effective
In August, hospitals across the country were penalized with Medicare reimbursement cuts due to high 30-day readmission rates. Affected facilities included 51 Wisconsin hospitals and 15 Utah hospitals. The potential to reduce these rates so that healthcare facilities can avoid federal penalties has made telehealth services a financial priority.
Healthcare provider TripleCare was the subject of a study offering further evidence of potential telehealth cost savings. The study, conducted by the TRECS Institute, found that TripleCare’s virtual physician services had both increased care quality and averted 91 unnecessary admissions. The result was more than $1.3 million in Medicare savings.
According to the press release, “Results revealed positive increases in net revenue for the study facility, which significantly exceeded the cost of TripleCare’s services, thereby improving both top- and bottom-line financial performance.”
Telehealth service adoption can provide patients and healthcare facilities in rural areas with other cost benefits as well. NTCA–The Rural Broadband Association released a report in March that estimated the average annual cost savings per medical facility could add up to:
- $5,718 in patient and caregiver travel expenses
- $3,431 in lost wages for time away from work to seek treatment
- $20,841 in hospital costs to retain highly trained staff
With many rural areas facing a shortage of specialists, telemedicine enables individual doctors to reach more patients. And the cost to patients for telehealth consultations is often lower than an in-office visit. In addition, telehealth reduces the time physicians might otherwise have to spend traveling to different facilities to meet with patients who are unable to travel. And, by enabling doctors to see more patients in a shorter amount of time, healthcare organizations can cost-effectively grow their membership while increasing care quality and patient satisfaction.